Inflammatory Bowel Disease (IBD): Understanding and Managing the Condition
Introduction:
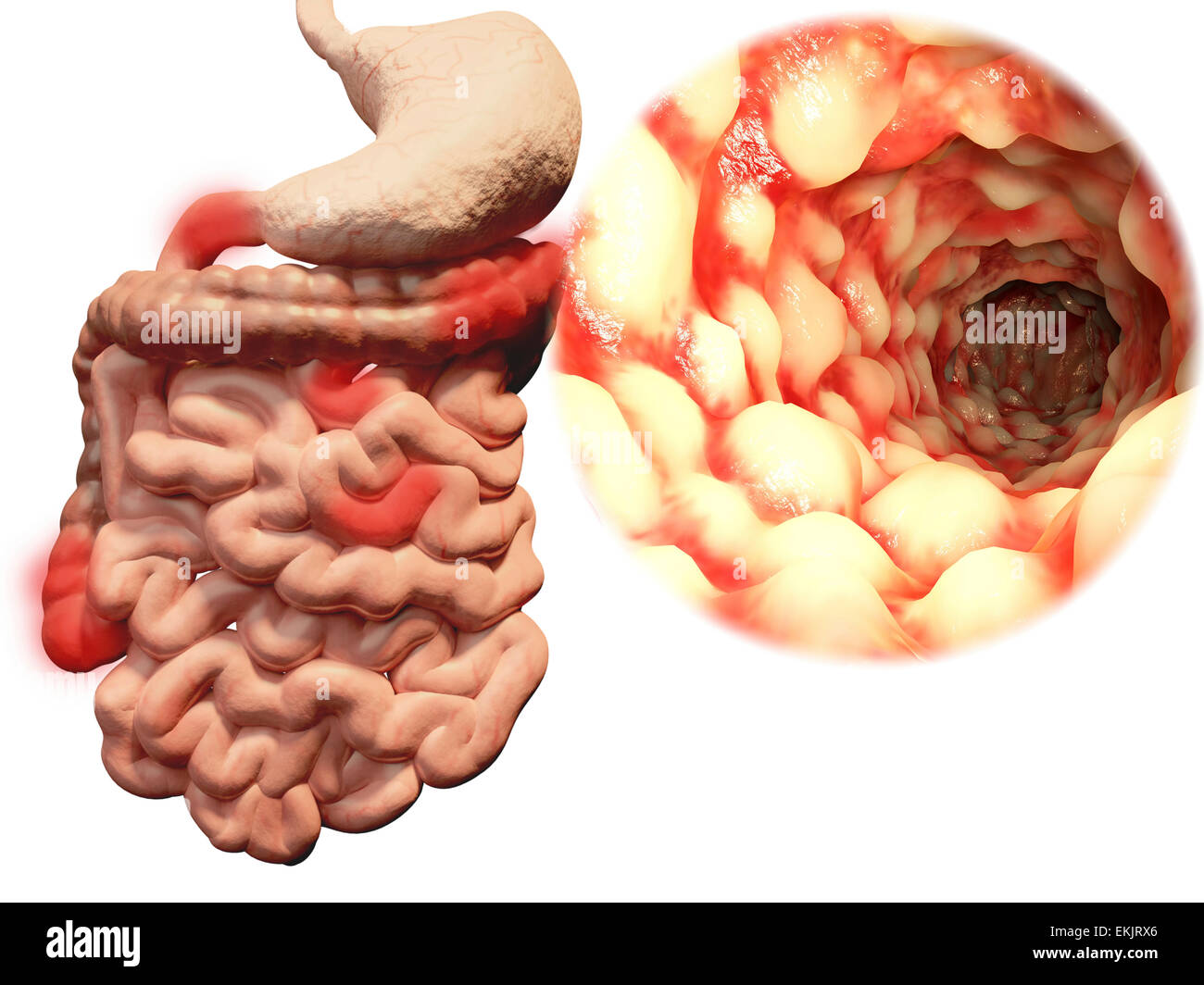
Inflammatory bowel disease (IBD) is a group of chronic disorders that affect the digestive tract. It primarily includes two conditions: Crohn’s disease and ulcerative colitis. These diseases cause inflammation in different parts of the digestive system, leading to various symptoms and complications. In this article, we will delve into the details of IBD, its causes, symptoms, diagnosis, treatment options, and lifestyle modifications.
Understanding Inflammatory Bowel Disease:
1. Crohn’s Disease:
– Crohn’s disease can affect any part of the gastrointestinal tract from the mouth to the anus.
– The inflammation occurs in a patchy manner with healthy areas surrounding affected regions.
– Common symptoms include abdominal pain, diarrhea, fatigue, weight loss, fever, and rectal bleeding.
2. Ulcerative Colitis:
– Unlike Crohn’s disease which affects any part of the GI tract discontinuously; ulcerative colitis specifically targets the colon (large intestine) and rectum.
– Inflammation begins in the rectum and may spread continuously through different segments of the colon.
– Symptoms include bloody diarrhea with mucus or pus, urgency to have a bowel movement but without relief after doing so.
Causes and Risk Factors:
The exact cause of IBD remains unknown; however, several factors contribute to its development:
1. Genetic Predisposition:
– Individuals with a family history of IBD are at higher risk.
– Certain gene mutations have been associated with an increased susceptibility to developing these conditions.
2. Abnormal Immune Response:
– IBD is believed to be an autoimmune disorder where an overactive immune response attacks healthy cells in the digestive system.
3. Environmental Triggers:
– Smoking: Smokers have a higher risk of developing Crohn’s disease while non-smokers are at a higher risk of developing ulcerative colitis.
– Diet: Although diet alone does not cause IBD, certain foods can trigger symptoms and worsen the condition.
Diagnosis:
Accurate diagnosis is crucial for effective management of IBD. Diagnosis typically involves:
1. Medical History and Physical Examination:
– The healthcare provider will review symptoms, medical history, and perform a physical examination.
2. Blood Tests:
– Blood tests help identify inflammation markers, anemia, nutrient deficiencies, or other conditions that may mimic IBD symptoms.
3. Imaging Studies:
– X-rays, CT scans, or MRIs help assess the extent and severity of inflammation in the digestive tract.
4. Endoscopy:
– Colonoscopy or sigmoidoscopy involves inserting a flexible tube with a camera into the rectum to examine the colon’s lining.
5. Biopsy:
– During endoscopy, small tissue samples (biopsies) may be taken to confirm the diagnosis and rule out other conditions.
Treatment Options:
The goal of treatment is to reduce inflammation, control symptoms, improve quality of life, and prevent complications associated with IBD. Treatment options include:
1. Medications:
a) Aminosalicylates: These drugs target mild-to-moderate inflammation in both Crohn’s disease and ulcerative colitis.
b) Corticosteroids: They provide short-term relief from moderate-to-severe flare-ups but have significant side effects when used long-term.
c) Immunomodulators: These medications suppress the immune system to reduce inflammation.
d) Biologics: Targeted therapies that block specific proteins involved in inflammation; they are often prescribed for moderate-to-severe cases.
2. Lifestyle Modifications:
– Dietary Changes: Identifying trigger foods and avoiding them helps manage symptoms.
– Stress Management Techniques: Stress exacerbates IBD symptoms, so adopting stress-reducing techniques such as exercise, meditation, or counseling can be beneficial.
– Regular Exercise: Physical activity improves overall well-being and helps reduce inflammation.
3. Surgery:
– In severe cases where medications fail to control symptoms or complications arise, surgery may be necessary.
– Surgery involves removing the affected portion of the digestive tract and reconnecting healthy segments.
Living with IBD:
1. Diet:
– Although there is no one-size-fits-all diet for IBD, certain dietary modifications can help manage symptoms.
– Maintaining a food diary and working with a registered dietitian can help identify trigger foods and create an individualized diet plan.
2. Support Network:
– Joining support groups or seeking counseling provides emotional support and helps individuals cope with the challenges of living with IBD.
3. Regular Check-ups:
– Routine follow-ups allow healthcare professionals to monitor disease progression, adjust treatment plans if needed, and address any concerns.
Conclusion:
Inflammatory bowel disease (IBD) is a chronic condition that affects millions globally. While it poses significant challenges in daily life, effective management through medication, lifestyle modifications, and regular check-ups allows individuals to lead fulfilling lives. By understanding the causes, symptoms, diagnosis process,and available treatment options for IBD,Crohn’s Disease,and ulcerative colitis patients are empowered to take charge of their health and work towards managing their condition effectively.
Leave a Reply